Dental health and your cat’s happiness are linked together. Just like people, cats’ dental health is tied to their overall health. Lack of regular dental care causes pain and tooth loss, and increases the risk of severe systemic infections affecting the heart, liver, and kidneys.
By the time cats are 2 years old, 85% of them have some form of painful dental disease. The most common forms of dental disease in cats include (Reference 1)
- gingivitis
- periodontitis
- tooth resorption
- stomatitis
- broken teeth.
Dental Health and your cat’s happiness
Gingivitis
Gingivitis is an early stage gum disease caused by bacterial plaque buildup. It presents as tender and red gums – look for a redline where the teeth meet the gums. Treatment: professional teeth cleaning at your vet’s clinic and a home oral care plan ).
Periodontitis
Left untreated, gingivitis becomes periodontitis, a chronic bacterial infection of the tissues supporting the teeth – the gums, the bone forming the tooth socket, and the ligament that holds the tooth in place. The plaque buildup leads to inflammation, irreversible destruction of supporting bone, and eventual tooth loss.
Treatment: The plaque, both the visible, pottery-like accretions and that plaque below the gum lines, must be removed during a professional teeth cleaning at your vet’s. Tooth extraction maybe necessary; antibiotics are rarely used in the treatment of periodontitis (Reference 1).
Tooth Resorption
Tooth resorption is a common, painful dental condition. Statistics show that 20-60% of cats suffer from this malady. The cat’s body breaks down and absorbs the tooth and root, starting at the gum line. X-rays are necessary to confirm this, and show us problems both below and above the gumline.
Treatment: Extraction of affected teeth (Reference 1).
Stomatitis
Stomatitis is a severe, painful inflammation of the mouth and gums. Thought to be an improper immune response to oral bacteria, affected cats often lose weight and don’t groom themselves well. (Reference 1)
Treatment: Treatment typically involves partial or full mouth extractions.
Broken Teeth
If a fracture opens up the root canal, pain and infection can result.
Treatment: The affected tooth is usually extracted although a dental specialist can perform a root canal on feline canine teeth (fangs).
Dental health and your cat’s happiness are linked together. Even if your cat continues to eat, they could be suffering pain every day due to dental disease. Cats are masters at hiding pain. Caregivers may or MAY NOT notice jaw chattering, changes in the chewing behavior or connect changes in activity and play behavior to dental pain.
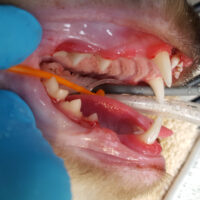
does your cat need those teeth to be happy?
Notice that most treatments for feline dental problems include extractions. While this may seem extreme, many of the options for humans such as filling cavities or implants, either don’t work or are just not practical for your cat.
Here are some questions raised by cat owners faced with extractions for their cat.
Is anesthesia necessary?
YES – Dental cleaning and surgery has to be done under general anesthesia because we use ultrasonic scalers and power drills in addition to hand instruments to clean and remove teeth. Even if the cat were to tolerate having their mouth open for an extended period of time, any small movement of their head could result in injury (Reference 2).
Are dental x-rays necessary?
Dental x-rays allow us to see what is happening above and below the gum line, allowing the veterinarian to determine whether a tooth needs extraction. Like human dentistry, a small film or sensor is needed to capture the images. Most cats will not tolerate having something wedged into their mouths when awake and x-rays must be done under anesthesia.
Will my cat be able to eat dry food after extractions?
YES. Cat’s teeth are different from human teeth: cats are carnivorous and are designed to eat primarily meat. Their teeth are designed to slash and slice; they do not have the flat surfaces that humans and other omnivores have to grind food. They often swallow small pieces of food whole and are able to eat kibble with fewer or no teeth (Reference 3).
Will my cat’s jaw be more prone to fracture after extractions?
After extractions, the tooth roots will not longer be there to stimulate the bone and the bone will recede. The jaw will temporarily be weaker but should stabilize once the bone heals. Leaving diseased teeth in place will result in more severe bone recession than a properly done extraction. The veterinary dentist may use a synthetic, bioactive ceramic bone graft material to fill sockets after tooth extraction, to maintain the jaw near “pre-extraction” height (Reference 3).
Oral surgery can be painful. Be sure to administer all your cat’s pain medication after surgery. If you are having difficulty, ask your vet if there are alternate forms of pain meds.
Dental health and your cat’s happiness are linked together. Treatment of the common dental problems suffered by cats often involves extracting painful teeth. Use of dental tools and the need to take dental x-rays requires the dental cleaning be done under general anesthesia. Most cats are able to eat dry cat food after having teeth extracted and proper dental technique minimizes bone loss in the cat’s jaws. Regular dental cleanings are the key to a healthy and happy life for your cat.
references
- Lobprise H Co-Chair, St Denis K Co-Chair, Anderson JG, Hoyer N, Fiani N, Yaroslav J. 2025 FelineVMA feline oral health and dental care guidelines. J Feline Med Surg. 2025 Nov;27(11):1098612X251398793. doi: 10.1177/1098612X251398793. Epub 2025 Nov 29. PMID: 41319038; PMCID: PMC12665832.
- The Feline Veterinary Medical Association (FelineVMA) and the Feline Oral Health and Dental Care Guidelines Task Force oppose anesthesia-free dentistry and endorse previously published position statements concerning anesthesia-free dental treatments (2025): https://avdc.org/PDF/Dental_Scaling_Without_Anesthesia.pdf
- Rochette J. Avoiding the “no”. Can Vet J. 2011 Dec;52(12):1361-2. PMID: 22654147; PMCID: PMC3215476.









 Unlike humans, who can place an inhaler between their lips, and breathe the medication in, the coughing cat with asthma, like young human children, must inhale the medication from a chamber.
Unlike humans, who can place an inhaler between their lips, and breathe the medication in, the coughing cat with asthma, like young human children, must inhale the medication from a chamber.






 Touch is important for many species. It is often part of a social interaction, cementing bonds between the members of a group. Primates (chimps, baboons,…) groom each other; dogs groom each other, birds preen each other as part of courtship or bonding. Domestic cats also groom and rub against each other in greeting.
Touch is important for many species. It is often part of a social interaction, cementing bonds between the members of a group. Primates (chimps, baboons,…) groom each other; dogs groom each other, birds preen each other as part of courtship or bonding. Domestic cats also groom and rub against each other in greeting.

 Sometimes, fear and anxiety can make it difficult for a cat to cope with her daily life. Perhaps there has been a change in the environment – a new cat or dog comes to live in the home or a new born baby comes home one day.
Sometimes, fear and anxiety can make it difficult for a cat to cope with her daily life. Perhaps there has been a change in the environment – a new cat or dog comes to live in the home or a new born baby comes home one day.